Annual Update Processes: The Charge Master & Beyond – Part 1
Annual Update Processes:
The Charge Master and Beyond – First Steps (Part 1)
It’s ‘that time of year’ – Time to review coding, payment system, and annual regulatory update rules that will be effective January 1, 2018. Here’s part 1 of a two-part excerpt from our 2018 CDM Update Educational Program to help with your update planning.
Consultants, Software Vendors, and Hospital Teams will all be busy from now until December working through a broad array of update information while ultimately ensuring stable and accurate reimbursement. Changes will impact numerous health care system departments and support areas. Complete and efficient update processes are essential to avoid claims delays, compliance risks, and revenue loss.
Who’s Doing What?
Annual updates require leadership, organization, and collaboration. Much of the new year’s data analysis is initially performed by Charge Management, Revenue Cycle, Coding, or Finance staff. Once all updates are released, structured strategic working sessions are performed with impacted technical, clinical, and support department representatives. Departments may need guidance on what is expected relative to the annual updates. Collaboratively, teams evaluate impacted charge items’ structure, charge protocol, pricing, and associated charge capture processes to ensure changes remain relative to cost and reimbursement. Administrative support will help keep the update program a priority.
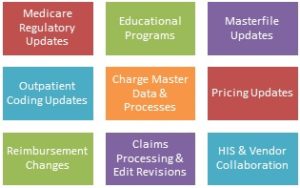
As we discussed in August’s First Steps for 2018 Charge Master Update Success, proactive Revenue Cycle and Charge Management teams have already begun their initial CDM update planning relative to the many areas noted in the graphic above. Beyond strategic planning, many have started analysis of changes that have already been released.
ChargeAssist® customers have already begun review of 2018 CPT-4® updates, 2018 AMA guidelines, and associated H&A auditor notes against their CDM data.
Upon release of 2018 outpatient Medicare payment system and edit changes in November, your vendors and consultants will compile data and release integrated change information. Aside from software updates, H&A will be attending the AMA CPT® Symposium in mid-November, and busy reviewing Medicare Final Rule details for key payment systems. Our in-depth 2018 Charge Master Update training manual, streaming department-specific educational webinar lectures, and other year-end materials will be released in our on-demand Annual Update Educational Program slated for access the morning of December 6th and available until late March 2018.
Your team will want to evaluate staffing, task ownership, education, leadership, and support in advance of the heads down work on your annual updates. The next section provides some updates for 2018 CPT-4® that will help with your planning process.
Implementation Planning for CPT-4® Coding
CMS and other payers utilize current-quarter CPT-4® codes for payment systems and claims edits. Current period CPT® codes are part of the approved Health Insurance Portability and Accountability Act (HIPPA) Transaction Code Set. Some CPT® codes will be hard-coded (i.e., populated in masterfiles), while others will be coded manually through HIM/Coder interpretation and assignment.
2018 American Medical Association (AMA) CPT-4® code updates have been available for several weeks in the change modules of the Holliday & Associates’ charge management software – ChargeAssist®. We have also posted the codes associated with the OPPS Proposed Rule data for preliminary reference to CMS’ proposed rates and status indicators. Once released, the Final Rule regulatory and payment system updates will need to be considered in tandem with CPT® to fully understand payment system impacts.
2018 CPT-4® contains updates that will require new charge development, charge item restructuring, and charge item repricing once CMS payment system and claims edits are finalized. Based on 4Q17 to 1Q18 CPT® files* there are 295 CPT® code-specific changes:
- 135 New Codes
- 86 Deleted Codes
- 58 Revised Code descriptors with content changes
- 16 Revised Code descriptors with only grammatical changes
*Note that AMA change totals in their published codebooks will vary due to data releases and publication cycles. Additionally, note that H&A only identifies ‘Revised Codes’ as those with modifications to the code descriptor.
Confirm that all team members and department representatives fully-understand AMA resources whether within the CPT manual or integrated into charge management tools such as ChargeAssist®.
- Ensure departments understand the codes and code sections that apply to their masterfiles.
- Consider updates to code sections as well as revisions to introductory guidelines within coding resources.
- The CPT® Professional manual displays changes in a green font.
- Arrow symbols (< >) surrounding verbiage are used to show new or revised text.
- The CPT® Changes publication from AMA explains all code book revisions. Look for their ‘rationale’ that summarizes the reason for the updates.
- Symbols in CPT® define new and changed codes, and there is always a note for deleted codes.
- Coding parentheticals or exclusionary parentheticals (following code descriptors) often define charge capture rules and require consideration when using the associated codes.
- AMA coding updates are listed in Appendix B of the CPT® manual and available to ChargeAssist® subscribers now. However, more strategic charge-specific reference information is listed in the ChargeAssist® Auditor Notes within the change modules. (We’ve had hospitals tell us that they saved 40-60 hours of research time annually using our summaries of the changes. Be sure to consider the Auditor Notes fields if you’re a ChargeAssist® subscriber.)
- Often, AMA may restructure codes or code families which may require a different charge structure, price, or charging protocol. This is true for numerous codes in 2018 and will require update of not only CDM data, but also the mapping of ancillary and order entry files to ensure correct charge capture.
- Remember that CPT® identifies any resequenced codes with a # symbol and may also change code numbering within a family of codes to accommodate the annual revisions. It’s become increasingly difficult to look at changes in numeric order alone.
Changes Beyond CPT®
While CPT® codes are critical for hospital and physician annual charge updates, there is other integrated information from Medicare that must be considered. Various payers’ coverage rules, payment methodology, and reporting requirements also help define which codes should be included in health system charging masterfiles and what rules should be established for claims accuracy.
The annual update team needs to ensure accurate CDM data population strategies based on your unique systems, masterfiles, payer, and operational environment. Despite transaction code set standards, there are still some limited payers that don’t accept new codes on January 1st. Check payer websites for their 2018 code acceptance timeline.
Once all data is released, it’s time to look at how masterfiles and processes will be affected. While it helps to see which charge items are impacted through your CDM tool, remember that your team will need to consider all codes with changes to confirm whether they may be applicable. Consider all aspects of a code’s changes to decide on file update strategies including: regulatory updates, HCPCS Level II code overrides, reimbursement rates, and associated payment and claims edit indicators. Note the relationships between new, deleted, and revised codes in both CPT® and HCPCS Level II across multiple coding sections. And finally, evaluate how updates to coding guidelines, payment system regulations, and edits may impact codes before making masterfile changes.
Summary
These annual update tips are early October tasks your team can conduct as you begin 2018 CDM updates. Part 2 of this series provides suggestions for mid-October to help teams craft a more comprehensive and coordinated annual update work plan.
We’re scheduling ChargeAssist® demonstrations now for teams ready for a new software solution for 2018 updates. Please call our office if you’d like to set up time and we can discuss your organization’s specific needs. Also, your team may wish to consider our 2018 CDM Update Program. It is free to ChargeAssist® customers and available for registration now at the following link: Holliday & Associates 2018 CDM Update Educational Program
Copyright Holliday & Associates 2017
And for more articles:
Annual CDM Update Tasks Your Team Can Easily Miss
Department CDM Update Internal Evaluation
Charge Master “spring cleaning” tips
Annual Update Processes: Build a Work plan that Really works
Annual Update Processes: The Charge Master & Beyond
